Filter :
जब जीन्स की बनावट में आनुवंशिक बदलाव (जेनेटिक म्यूटेशन) आता है तो कोशिकाएं सामान्य से असामान्य हो जाती है जो आगे जाकर कैंसर का कारण बनती हैं। जब गुदा की नली में मौजूद कोशिकाओं में आनुवंशिक बदलाव आता है तो इसे मेडिकल की भाषा में गुदा का कैंसर यानी एनल कैंसर कहते हैं।
गुदा कैंसर की गंभीरता को ध्यान में रखते हुए इसे चार चरणों में बांटा गया है। सिटी स्कैन, एमआरआई और पेट का स्कैन करके डॉक्टर गुदा कैंसर के चरण का पता लगाते हैं। कैंसर के अनेक कारण हो सकते हैं जैसे कि:
गुदा कैंसर होने पर आप खुद में अनेक लक्षणों को अनुभव कर सकते हैं जिसमें मुख्य रूप से मलाशय यानी रेक्टम या गुदा से खून निकलना, गुदा के आस-पास के क्षैत्र में दर्द महसूस होना, गुदा की नली में असामान्य मांस बढ़ना और गुदा में खुजली एवं असहजता महसूस करना आदि शामिल हैं।
अगर आप ऊपर दिए गए किसी भी लक्षण को खुद में अनुभव करते हैं तो बिना देरी किए कैंसर विशेषज्ञ से परामर्श करना चाहिए ताकि समय पर इसका निदान और उपचार करके इस बीमारी को हमेशा के लिए दूर किया जा सके।
गुदा कैंसर के चरण और गंभीरता की पुष्टि करने के लिए डॉक्टर गुदा के कैंसर का निदान करते हैं। निदान की इस प्रक्रिया में निम्न जांच शामिल हो सकते हैं:
इस जांच के दौरान, डॉक्टर एक दस्ताना पहनते हैं, अपनी उंगली को लुब्रिकेंट से चिकना करके उसे रेक्टम यानी मलाशय के अंदर प्रवेश करते हैं। उसके बाद, गुदा की नली और रेक्टम की असामान्यताओं की पुष्टि करते हैं। गुदा का कैंसर होने पर डॉक्टर रेक्टम में कुछ असामान्य मांस का बढ़ा हुआ टुकड़ा महसूस कर सकते हैं।
इस जांच के दौरान डॉक्टर एनोस्कोप नामक मेडिकल उपकरण का इस्तेमाल करके गुदा की नली और रेक्टम के आंतरिक हिस्सों की असामान्यताओं की जांच करते हैं। एनोस्कोपी के दौरान डॉक्टर एनोस्कोप नामक मेडिकल उपकरण का इस्तेमाल करते हैं। एनोस्कोप एक पतली ट्यूब की तरह होता है जिसका एक छोर पर छोटा सा कैमरा और लाइट लगा होता है।
गुदा में कैंसर का निदान करने के लिए डॉक्टर अल्ट्रासाउंड भी करते हैं। अल्ट्रासाउंड के दौरान डॉक्टर गुदा के आंतरिक हिस्सों की तस्वीर प्राप्त करते हैं जिससे उन्हें गुदा की असामान्यताओं को समझने में मदद मिलती है।
ऊपर दिए गए जांचों में गुदा में असामान्यताएं पाने पर डॉक्टर उत्तकों का एक टुकड़ा निकालकर बायोप्सी जांच करने के लिए लैब में भेजते हैं। माइक्रोस्कोप की मदद से जांच करके इस बात की पुष्टि की जा सकती है उस उत्तक में कैंसर होगा या नहीं।
गुदा में कैंसर के चरण, गंभीरता और मरीज की उम्र एवं समग्र स्वास्थ्य को ध्यान में रखते हुए डॉक्टर अन्य जांच करने का भी सुझाव दे सकते हैं। जांच के परिणाम, गुदा कैंसर के चरण और मरीज की समग्र स्वास्थ्य को ध्यान में रखते हुए डॉक्टर उपचार के प्रकार और पद्धति का चयन करते हैं।
अगर आप खुद में गुदा कैंसर के लक्षणों का अनुभव करते हैं या आपको इस बात का शक है कि आपको गुदा कैंसर है तो आप हमारे कैंसर विशेषज्ञ के साथ परामर्श कर अपनी बीमारी का सटीक जांच और उपचार करा सकते हैं।
कैंसर विशेषज्ञ का मानना है कि समय पर गुदा में कैंसर का निदान होने पर उपचार के सफल होने की संभावना बढ़ जाती है। हमारे विशेषज्ञ के साथ अपॉइंटमेंट बुक करने के लिए आप इस पेज के ऊपर दिए गए फोन नंबर या बुक अपॉइंटमेंट फॉर्म का उपयोग कर सकते हैं।
हाँ. समय पर गुदा कैंसर का उचित जांच करके सटीक और सफल इलाज संभव है। लेकिन अगर यह अपने आखिरी चरण में चला जाए और लक्षण गंभीर रूप ले लें तो उपचार में बाधाएं पैदा हो सकती हैं। विशेषज्ञ का कहना है कि गुदा कैंसर के लक्षण अनुभव होने पर जल्द से जल्द कैंसर विशेषज्ञ से परामर्श करना चाहिए ताकि इसकी गंभीर जटिलताओं के खतरे को कम या ख़त्म किया जा सके।
Congratulations! You have entered the third trimester of your pregnancy! It is amazing how you have been able to overcome some of the most testing phases of your pregnancy journey. Now, all we do is make sure we welcome the baby in the most healthy and happy way. Your pregnant belly is booming and you are glowing in anticipation with the happy pregnancy hormones doing their job.
This is also a time when you and your family start planning for the actual delivery. How to choose a birthing plan? How to remain agile during this phase? What are the best sleeping positions? How to ensure breastfeeding is properly done? For that here’s a brief guide on how to prep for your delivery How to prep for your delivery?
But in the third trimester, what are the problems pregnant women need to deal with? What should you eat, what should you avoid, there are a whole lot of questions you need answers to. Don’t worry, just read on…
The third trimester is more tiring and uncomfortable than the other two trimesters primarily because the embryo grows to its full form. The discomfort is mainly attributed to the baby’s position and size, and with the due date approaching soon, anxiety also reaches its peak, making this trimester emotionally challenging as well. It is very important that at this stage you remain positive and try to adapt to the upcoming changes. Here is what you can expect during this stage:
Apart from this adequate prenatal care should be taken w.r.t. Your babies, such as checking the baby’s progress in terms of size, heart rate, position and movements. Make sure you and your gynaecologist have chalked out a proper birthing plan and made your choices.
There are various aspects that need to be considered for a delivery. While in the earlier days one had midwives and home deliveries, now we look for options where the pain and medication for the pregnant mother is well managed for a smoother and natural delivery. For this one needs to choose the right healthcare partner. With professional help the following concerns will be addressed:
Make a checklist of all the things you will need during your third trimester. Start with charting out a birthing plan with your OB-GYN and healthcare provider. This will include monitoring your health pre-labour, any concerns that may indicate a c-section and consultations post-delivery.
At the CK Birla Hospital®, we take pride in planning things out for our expectant families for a seamless and memorable experience of welcoming a child into this world. For this, we don’t leave any stones unturned.
Everyone who sees you now is extra careful around you and more attentive to your needs. This is by far the second-best feeling during a pregnancy trumped only by the news of the baby’s arrival. But like they say, “with great power comes great responsibility”. This is why, our hands-on team of professional caregivers make sure you are well supported and looked after in a homely atmosphere, under compassionate care. Check out our comprehensive maternity packages, including attractive offers and discounts, now available at the CK Birla Punjabi Bagh.
We often come across this very common phrase of “giving the cold shoulder”. The phrase implies someone deliberately ignoring the other by not moving in their direction or by snubbing them by showing their back. The origin of the phrase lies in a medical condition called adhesive capsulitis, popularly called the frozen shoulder.
This is a very common condition and cases of frozen shoulders spike up, especially around winter. This is also a very common sports injury, especially among people around the age of 40 years. This condition is primarily characterised by stiffness in the joints and pain when trying to mobilise the pain. But what leads to a frozen shoulder? What are its symptoms? How can you get rid of it? To get answers to all possible questions w.r.t. Frozen shoulder, read on…
Table of Contents
Medically referred to as adhesive capsulitis (AC), a frozen shoulder is when your shoulder develops stiffness and reduces the mobility of your shoulder joints. It hurts to move the shoulder joint. Over a period ranging between 1 to 3 years, the symptoms get better and the condition heals completely.
This condition develops when the shoulder remains in one position for a long time. It is often seen developing post-surgery trauma injuries caused on the arm. It can be treated through physiotherapy exercises, corticosteroid medication, injected pain medication and in extreme cases arthroscopic surgery. The main purpose is to release the stiffness in the joint.
Usually, this condition is found more in women than men. It does not recur in the same shoulder, however, one can have a recurring case if treatment is not done properly. The pain might move from one shoulder to another in some circumstances.
You Can Also Read: Shoulder osteoarthritis – symptoms, causes & treatment
Let us first understand how a normal shoulder works. Our upper arm, collar bone, and shoulder blade, together with tendons and muscles form the shoulder capsule. Synovial fluid in this capsule lubricates the joints for easier movement.
Now for a person with a frozen shoulder, this capsule thickens and becomes stiff. These tissues develop adhesions and the synovial fluid is lowered. Finally, this leads to a stiff shoulder capsule and a frozen shoulder.
While the above is the mechanism of a frozen shoulder, there are no clear-cut symptoms of frozen shoulders. However, one can understand that they are developing the condition by being aware of the stages of a frozen shoulder.
Typically, a frozen shoulder develops gradually, in three distinct stages.
In this stage, any slightest motion or movement of the shoulder and shoulder joint causes pain and restricts mobility. This stage builds over time with more and more restricted movements and lasts between 2 to 9 months without treatment.
At this stage, the pain might be lesser since the body has developed a pain threshold over time. However, the shoulder stiffness grows severe making mobility far more difficult. This stage, if not treated, lasts between 4 to 6 months. For those who experience more pain, the condition worsens at night, often disrupting sleep.
Post-treatment at this stage, your shoulder’s mobility starts improving. This stage lasts from 5 to 24 months, till the normal range of motion in the shoulders is restored.
You Can Also Read: Shoulder Arthritis – All You Need to Know
The primary cause of a frozen shoulder is stiffness of the shoulder. As explained earlier, the shoulder capsule includes connective tissue lubricated by the Synovial fluid. When the capsule thickens, lubrication depletes and tissues tighten, the frozen shoulder occurs restricting shoulder movement.
The above-mentioned series of events can be linked to:
Based on these causes we can profile the risk factors associated with this disease.
The people who are at a greater risk of developing a frozen shoulder can be profiled under the following categories:
Your orthopaedic will focus on your pain relief and might suggest a combination of anti-inflammatories or steroid injections with physical therapy to restore shoulder motion.
Shoulder manipulation can also be performed under general anaesthetic to release the stiffness. Another way to release a stiff shoulder is via Hydrodilatation. In this case, along with steroids, sterile water is injected into the joint capsule to stretch the tissue and restore the mobility of the joints.
Apart from medication, a physiotherapist will suggest the following exercises for each of the three stages of a frozen shoulder:
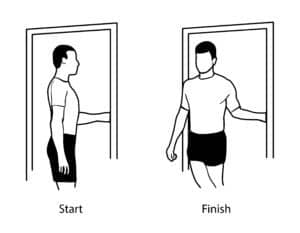
Stage: Freezing
Difficulty: Medium
Procedure: Stand in a doorway. Bend the arm of your affected shoulder 90 degrees and hold one of the sides of the door (as shown in the first image). Now keep your hand in place (as shown in the second image) and rotate your body. Hold the pose for 30 seconds. Relax. Repeat.
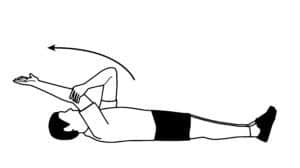
Stage: Frozen
Difficulty: Medium
Procedure: Lie on your back with your legs stretched out. Use the arm of your unaffected shoulder to lift your frozen shoulder’s arm overhead. Keep extending the arm till you feel a gentle stretch. Hold for 15 seconds. Relax and slowly return to the starting position. Take a few relaxing breaths and repeat.
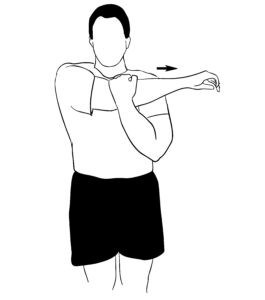
Stage: Thawing
Difficulty: Medium
Procedure: Carefully pull an arm across the chest and bring your shoulder under your chin as much as possible. Hold the pose for 30 seconds by breathing in and out. Relax and return to the original pose. Take another breath and repeat.
These stretches will not only help you with a frozen shoulder but also help you prevent any pain or stiffness in your shoulders when you practise them regularly.
In case none of the above gives any respite from the pain, surgery is the ultimate treatment. Here the problem area is approached using arthroscopy, and the scar tissue is removed to eliminate stiffness and relieve the pain completely. However, this is resorted to in rare cases.
Essentially the frozen shoulder is a type of inflammation which makes everyday tasks tedious. The longer it is left untreated the slower the progress w.r.t. the pain. While we cannot confirm whether you will get a frozen shoulder or not, we can take the following preventive measures:
Apart from this, it is always advisable we don’t ignore our body’s cry for help. If you experience any prolonged discomfort, do reach out to the Department of Orthopaedics at the CK Birla Hospital. Our award-winning team of seasoned professionals have a proven track record of handling a diverse variety of orthopaedic conditions with precision and care. To book a consultation simply walk in or call +91 124 4570112
Frozen shoulders often take a while to fully recover. The best route is physiotherapy where we perform a few exercises regularly in different stages of the frozen shoulder. Another cause of frozen shoulder is thyroid and diabetes, which can be controlled through lifestyle changes. For all other treatment options, complete recovery takes up to a full year.
Winter is already knocking at our doors and the season of ice-cold winds is here! However, a drop in the temperatures often worsens bone-related issues. While these complications are the worst in senior citizens, people of all ages should stay a little extra cautious about their bone health during winter.
Most orthopedic surgeons suggest specialized care for their patients during winter. Some of the best orthopedic doctors in Gurgaon practicing at CK Birla Hospital and have started dedicating more time to providing additional tips to their patients, helping them keep their bones healthy in winter.
If you are looking forward to enjoying the season and keeping your bone health intact, here are a few important tips for healthy orthopedic care in winter:
Table of Contents
During winter, mobility is the key to maintaining your bone health. Do not keep your body still for too long. People often feel extremely lazy during winter and tend to spend a lot of time huddled in their blankets. However, low-impact activity affects your joints and makes them susceptible to various complications.
Even if you are not willing to leave your house, it is advisable to keep your limbs mobile by walking around in your room, using your treadmill, or indulging a little more in your daily chores.
Sweets taste best during winter! However, the pain of joint surgery is equally painful. Prevent your body from putting on additional weight during the winter. Maintain a healthy body weight according to your BMI throughout the season to keep your bones healthy. Additional weight puts extra pressure on your bones.
Especially if you are over 40 years of age, it is very important to check the unhealthy winter weight gain. As the winter has set in, dieticians around the world have started spreading awareness by seeking healthcare marketing services about maintaining a healthy weight.
Especially if you are going out in the cold weather, make sure you keep your hands and feet covered. Keeping them warm and cozy prevents your bones from bearing the brunt of the season. Even if your bones are slightly weak or recovering from an injury, they start aching when exposed to a cold environment.
It is advisable to leave your house wearing gloves and socks. If you are driving, you can keep a pair of gloves in your car. Warm clothes act as good insulation and help you keep your bones healthy.
If you already suffer from bone or muscle-related issues, keeping your senses calm during the winter is important. You must have noticed people (especially older) complaining about their joint aches getting worse during winter. This is because stress contracts your muscles and makes your bones stiff.
This involuntary response makes your bones vulnerable and worsens the issues you already have. A lot of people prefer applying ointments or muscle pain creams to achieve a calming effect. You can also take a warm bath to stay calm and composed during the winter.
Contrary to popular belief, drinking plenty of water is equally important during summers and winters. Dry air often makes you feel dehydrated too quickly. Keep yourself dehydrated by drinking water at room temperature or making yourself a hot cup of tea.
The amount of water you drink affects how your bones function. Water carries calcium and other healthy nutrients to your bones, keeping them healthy. In a season when your bones are already more susceptible to issues, it is advisable to prevent your body from getting dehydrated.
Winter is a season when you may experience a lot of unhealthy cravings and experience multiple temptations. However, if you want to keep your bones healthy, it is important to keep your diet healthy and balanced.
Include a variety of foods like leafy vegetables, fruits, lean meats, and whole grains in your diet to ensure healthy bones. Try your best to steer away from processed foods that are high in saturated fat and sugar. Along with keeping your bone health in check, eating a healthy and balanced diet will prevent you from getting obese.
If you are older or are dealing with bone-related issues, it is advisable to consult your orthopedic doctor about the need for supplements during winter. Some doctors suggest increasing the intake of vitamins like vitamin D and K once the weather gets cold. Make sure you take such supplements only after being advised by your doctor.
While getting out of bed feel like the worst thing to do on a winter morning, early morning exercises can work wonders for your bones during winter. As discussed earlier, mobility is important to ensure sound bone health. When you exercise, your blood flow, heart rate, and breathing improve. Exerting a little extra pressure on your bones makes them tougher and more resistant to various health complications.
Ideally, healthcare experts recommend 30 minutes of low-to-medium intensity workout every morning to keep your bones and muscles healthy. Along with keeping you safe from bone-related diseases, this also helps you stay in shape by the time you hit the beach in the summer!
You must have seen people who enjoy alcohol use its warming tendency as an excuse to drink more during the winter. Know that alcohol hampers your bone density and increases the chances of osteoporosis. Make sure you refrain from excessive alcohol consumption just because it has a warming effect on your body.
These were some of the most important tips for effective orthopedic care during the winter. While enjoying the season and everything that it brings along, make sure you do not take your bone health for granted. If you feel even slight abnormalities or meet with an accident you think has damaged your bones, seek immediate help from your orthopedic.
ACL tears can be extremely painful and the last thing you would want for a sports injury! Along with restricted mobility and physical trauma, ACL tears often make patients feel as if they will never completely recover from the damage.
However, that is certainly not the case. Holistic ACL tear surgeries help patients heal their ACLs and get back on the field in no time. Having said that, it is important to heal the right way. After ACL surgery, patients are recommended extensive rehabilitation to let their limbs get used to normalcy in a slow and sustainable manner.
ACL (anterior cruciate ligament) is an important ligament in your body that connects your thighbone to your shinbone. ACL tears commonly occur due to sports injuries where players tend to damage their ACL by suddenly stopping, changing directions, jumping, or landing in a crude manner. Most players feel a “popping” sensation near their knees or hear an audible “pop” sound followed by excruciating pain. If you have had your ACL surgery done recently, here are a few tips that should help you ease your recovery.
Table of Contents
Like most bone and muscle injuries, ACL tear results in the swelling of the area around your knee. It is your body’s inflammatory response to the trauma of the injury. While you recover, make sure you reduce the swelling by applying ice packs, wearing a Tubigrip sleeve, and keeping your knee at rest.
Applying ice is arguably the most effective cure for swelling after ACL surgery. Ideally, orthopedics advise three to four daily sessions of 15 minutes each to ease the swelling.
If you have gotten an ACL tear surgery done, you cannot ignore the fact that you will be in physical pain for some time. This pain may prevent you from performing exercises essential for your recovery. To control postoperative pain, you can take painkillers as advised by your doctor before performing the necessary exercises. However, make sure you stick to the dosage recommended by your doctor (acl tear doctor). Never make the mistake of taking painkillers every time you experience pain in the affected region.
Restoring full leg straightening is an important part of the ACL surgery recovery process. You need to get your leg straightened up to restore its impaired mobility. To achieve the desired results, it is necessary to bear some pain and keep the swelling under control. Doctors always recommend doing extension stretch exercises throughout the day to ease into a complete recovery.
If you are sitting at rest or lying on your bed, you can straighten out your leg with its heel propped on a pillow to force it straight. Low-load and long-duration stretch exercises help you strengthen your leg effectively. Make sure you don’t keep your leg bent. Avoiding full straightening can lead to a permanent limp.
Doctors often advise tracking the progress on a weekly basis. After the sixth week, you should be able to stretch your leg enough to mimic normal functioning. With the help of healthcare SEO services, several orthopedics do their best to educate people about the importance of full straightening.
To attain complete mobility of your leg back, keep bending your knees as you recover from ACL surgery. Most patients are able to bend their knees after the surgery without any difficulty. Also, it is safe to bend your knees after an ACL surgery to ensure holistic recovery. Most physiotherapists help patients get onto the CPM machines one day after their ACL tear surgeries.
This is why the rehabilitation period is important to patients to restore the complete mobility of their limbs. It is common for patients to feel as if this would damage their recovery process. This is certainly not true. In fact, knee-bending exercises help you recover in a holistic and systematic way.
Kneecap pain is arguably the most painful symptom of ACL surgery. While some patients tend to damage their kneecaps along with their ACLs, most cases of kneecap pain are due to secondary causes. The tightness of the tissue located on the outer half of your knee weakens, making your kneecap vulnerable and susceptible to pain. Doctors recommend ITB (IT band) massage to relieve the pain in the kneecap. If the band seems too tight, you can do some ITB stretches or an ITB roller.
The quadriceps muscles located in front of your thigh form the biggest muscle group in your body. These are the first muscles that waste away during an injury. On average, for every week of quadriceps wastage, it takes six weeks to recover.
Considering the time it takes for your quads to heal, make sure you start working on them as soon as possible during your recovery period. This will speed up your recovery and prevent your quads from wasting away anymore. Straight leg raising is the best way to deal with healing your quadriceps.
As simple as it sounds, walking plays a very important role in ACL recovery. Your legs need regular movement to get back in shape and recover fully from the damage. You may require crutches and other external support for the initial few days, but you will soon be able to walk on your own.
Every step you take will contract your quadriceps, calf muscles, and hamstrings, thereby restoring the normal functioning of your body.
ACL tears and surgeries can be really painful and tedious. It is important to understand that recovery and rehabilitation are as important as the surgery itself. Make sure you follow these steps to ease into recovery mode and get back to normalcy.
Moreover, make sure you seek medical help whenever you encounter a problem you don’t have a solution for. Stay in touch with your orthopedic doctor and physiotherapist to ensure perfect recovery and return to your life with a healthy knee.
It is that time of the year again when the temperature outside is low, the humidity levels have hit rock bottom and everything feels dry. This dryness is not just reflected in the atmosphere but also on the surface of our skin. With this dryness comes the familiar seasonal concept of itching and flaking of the skin. Itchy skin can be very irritating. It makes you want to scratch non-stop. So out comes the bottles of moisturisers and body lotions that can help soothe the itch.
Itchy skin can be intense. The more you rub or scratch, the itchier it becomes, leading to the urge to scratch. Up to a certain extent we all end up with an itch or scratch. But breaking this itch-scratch cycle becomes difficult. In such cases, you need to get proper medical attention to solve the problem from the root cause. Depending on the cause, and the frequency of scratching, your skin may appear normal, rough, bumpy or red. Sometimes the skin might end up bleeding or become infected. None of which is desirable. So to understand what needs to be done and how to cure itchy skin
Table of Contents
Medically, itchy skin is also known as pruritus (proo-RIE-tus). It can happen to anyone. It all depends on the cell regeneration speed of the individual. Dry skin problems are very common in older people since skin tends to dry faster with age owing to slower cell regeneration.
However, most of these instances deal with various self-care measures that we keep adopting from time to time. When you seek long-term relief you need to get it reviewed by a dermatologist. They will help treat the problem using medicated creams, oral medicines and moist dressings.
Skin is universal in our bodies. So dryness-induced itchy skin can affect the smallest areas, like our scalp, arms or legs, or in worst-case scenarios the whole body.
With itchy skin sometimes there are no noticeable changes or symptoms apart from itchiness. However, other visible signs can be redness, cracks, scratch marks, leathery/scaly patches, bumps, spots or blisters.
You must show your condition to a dermatologist when
If it does not respond to a dermatology treatment, it has to be forwarded to an internal medicine expert to understand the underlying concerns that are leading to this dryness.
There can be various causes due to which you can end up with itchy skin. These are:
Any other cause might just be incidental to any side effects caused by medication or hand-foot-mouth disease which is triggered by consuming chemical compounds your body is not friendly with.
Also Read: 8 Signs Your Liver Is Healing
Prolonged itching and persistent scratching can increase the severity of the itch, leading to infection and scarring.
| Cause | Effect | Relief |
| Extremely dry skin | Intensely itchy | Medicated moisturiser |
| Bug bites (mosquito, bed bugs, lice, ringworms and mites) | Itch can be long-lasting and uncontrollable, except in the case of mosquitoes | Topical itch relief ointments |
| Diseases like dermatitis, chickenpox, eczema, folliculitis, hand-foot-and-mouth disease, psoriasis, neurodermatitis, hives, ringworm, (herpes) shingles, and others | Prolonged uncontrollable itching and rashes | Depending on the cause the relevant disease specialist needs to be consulted for the right treatment |
To understand the various modes of prevention, we need to first profile the group of people who are more susceptible to getting the problem in the first place. While anyone can suffer from pruritus, the following need to be extra careful:
Now that we know who is most at risk, we can approach each concern independently. The entire treatment depends on the cause. If it is a drug reaction then itching will be accompanied by rashes. But all other itches are mostly dependent on our skin’s hygiene. So here is a checklist that will keep you protected for longer.
If these kinds of things keep happening to you often and/ or you have similar symptoms that keep affecting your skin in the long term, then it is advisable to seek medical intervention from a professional dermatologist. At the CK Birla Hospital, our derma specialists are known to isolate each case and give customised treatment plans to relieve derma problems in the long term. If there are other aspects involved, the internal medicine team will also be involved. But it all starts with you reaching out to us. Walk in or book an appointment here.
Pruritus is itchy skin which can be linked to a variety of different causes, both severe and trivial. Urticaria on the other hand is a skin condition that ends up causing hives and gives a tickling or burning sensation in some areas of your skin. Therefore urticaria is a bigger concern of which a symptom is pruritus.
Sporting events demand a lot of physical exertion from each player. With repeated workouts, practice sessions, and above all stress, in innumerable instances, an unfortunate turn of events leads to a lingering sports injury that takes away months of hard work in a wink. Double Olympic and World 800m record holder, athlete David Rudisha was benched for 16 weeks after he twisted his ankle at home which turned out to be a fracture. English Cricketer Jonny Bairstow had to miss out on the T20 World Cup last year due to a broken fibula bone fracture after a freak accident.
Closer home double Olympic medallist shuttler PV Sindhu bowed out from the World Tour Finals due to a stressed ankle injury. And at this year’s ongoing Football World Cup Group match Neymar’s pesky ankle injury sent the whole world into a frenzy about Brazil’s chances of winning the cup. An ankle fracture can change fortunes not just for a player but also for an entire country. While these hits and misses are a part of the process, let us understand the impact and extent of the injury on our bodies.
Table of Contents
A broken ankle signifies one or more of the bones that make up the ankle joint are broken. It can be of different types:
In the latter, it may lead to disabling movement. Mostly it is advised that you do not put weight on your ankle for a few months, which is why you have restricted movements w.r.t. walking, driving, playing sports, and overall work.
The ankle joint is made up of 3 bones: the shinbone (tibia), the smaller bone of the lower leg (fibula) and the small bones in between the heel bone (calcaneus), tibia and fibula.
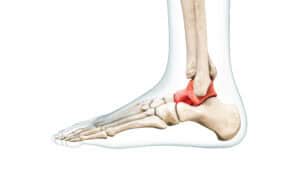
Apart from these, there is the Medial malleolus at the end of the tibia on the inner end of the ankle. The posterior malleolus is behind the tibia and the Lateral malleolus is the prominent bone at the end of the fibula on the outer side of the ankle. All of these share the ankle joint which gives mobility to the ankle and the syndesmosis joint which provides stability.
Orthopaedic experts classify fractures based on the area broken or the part of bone displaced. The fracture at the end of the fibula bone will be called a lateral malleolus fracture. And if the tibia is also broken this will be called a bimalleolar fracture. Similarly, if a bone is displaced it is a displaced fracture and if the bone comes out through the skin it is called an open fracture.
Ligaments in our body connect bone to bone to build stability in the joints. When you get a sprain in your ankle, the ligament gets injured. If torn, it is linked to an adjoining fracture. The deltoid ligament, found on the inner part of the ankle, lends stability to the ankle. If it is torn the ankle becomes unstable.
In our ankle joint two or more bones are cushioned by a lining between the bones, called cartilage. If the cartilage starts thinning or damages the cushioning, it leads to arthritis or inflammation in the joint.
The main causes of a broken ankle are:
Based on the event that leads to the injury, broken ankles can be attributed to:
In the case of a broken ankle, the only symptoms are pain and swelling, either in the ankle region itself or spread towards the foot or knee. Although the symptoms for sprain are similar, in the case of a fracture, the pain will feel 100x more when the injured person puts weight on their ankle.
In order to ensure proper recovery, the first step is diagnosis. With the help of various imaging tests, the bone structure and point of impact can be ascertained for proper diagnosis. Your orthopaedic will suggest X-rays of the region, to ascertain whether the pain is due to a broken bone, soft-tissue injury or sprain. In case of a traumatic incident, other radiology imaging, like a CT scan or MRI will be suggested.
If the results confirm a fracture, immediately approach an orthopaedic surgeon. The surgeon will be able to tell you whether or not surgery is needed.
There are different types of ankle breaks. Some of these do not require surgery. But when they do, it is important that the surgery is conducted by a skilled foot and ankle specialist. Timely and appropriate surgical intervention will help the ankle joint heal effectively. A shoddily executed surgery in the long term can lead to further complications, such as:
The ultimate goal is to restore bone alignment and ensure stability in the ankle joint. A good orthopaedic surgeon will ensure that the broken bones heal as close to perfectly as possible. Since a malalignment of even 2mm may lead to arthritis. It is easier to heal fractures than treat arthritis.
Mild ankle breaks that are stable and have no displacement can be managed non-surgically with the help of a splint, leg cast, or walking boot. In cases where that is not possible due to the delicate placement of the mild fracture, patients are advised to use crutches to restrict the pressure from weight bearing. For serious fractures, where the bones or their fragments become misaligned, surgery is required.
You Can Also Read: Best Food for strong bones and joints
An ankle fracture, which does not involve surgical intervention, can heal on its own. Some of these are:
Postoperative care is highly essential in the case of orthopaedic surgeries, the same applies to ankle repair. A good orthopaedic surgeon will ensure minimal discomfort and maximum gains for the patient. Some precautions are necessary for patients to follow:
At the CK Birla Hospital, we use the latest surgical innovations to ensure every patient gets a shorter healing time but gets complete and effective recovery. This patient-centric approach not only helps the patients heal better but also ensures zero to minimal chances of postoperative complications. In case you are facing any of the symptoms do reach out to us, or book a direct appointment at the CK Birla Hospital.
Depending on the extent of the fracture, treatment is prescribed. For a full-blown fracture, the patient cannot walk before 6 weeks. And can only be allowed to walk when all their x-rays indicate full bone healing. Weight-bearing and walking would be gradual depending on the progress in physiotherapy.
If the fracture is non-displaced, then a sling or a cast is given to the patient for basic mobility. However, walking can only start when the X-ray indicates complete healing and zero misalignments.
Yes. It will need a cast or splint if the recovery is non-surgical for up to 4 to 8 weeks, depending on the recovery as visible from subsequent x-rays. Without any complications, in 4 weeks the fracture heals enough to come out of the cast.
A fracture without misalignment or no fragments heals faster than a trauma fracture. So no, a fractured ankle is not worse than a break.
Walking after an ankle fracture is dependent upon the severity of the fracture. If it is a clean break it will take at least 8 weeks to heal properly to enable the patient to start walking wearing crutches or support. However, if the fracture is treated non-surgically, shows no alignment issue and subsequent x-ray shows complete healing, the cast can be removed. Walking is usually not advised before week 4.
हर किसी को मुलायम और खूबसूरत त्वचा पसंद है और इसके लिए लोग तरह-तरह के क्रीम, फेस पैक, लोशन और क्रीम का इस्तेमाल करते हैं। हालाँकि, कई बार इन सबके बावज़ूद भी त्वचा में रूखापन आ जाता है।
आमतौर पर त्वचा में रूखापन सर्दी के मौसम में आता है, लेकिन कुछ लोगों को गर्मी के मौसम में भी इस समस्या का सामना करना पड़ता है। त्वचा में रूखापन होने पर वह सुखी यानी ड्राई दिखती है।
कुछ मामलों में त्वचा का रूखापन त्वचा के फटने और उसमें खुजली या जलन का कारण बन सकता है। आइए, इस ब्लॉग में हम त्वचा में रूखेपन के कारण और उसके घरेलू उपचार के बारे में विस्तार से जानने की कोशिश करते हैं।
ये भी पढ़े: हर्पीस बीमारी क्या है? इसके कारण, लक्षण और उपाय
Table of Contents
त्वचा में रूखापन कई कारणों से हो सकता है जिसमें निम्न शामिल हो सकते हैं:
इन सबके अलावा, दूसरी स्वास्थ्य समस्याएं जैसे कि डायबिटीज, कुपोषण, हाइपोथायरायडिज्म और महिलाओं में मेनोपॉज एवं हार्मोनल असंतुलन के कारण भी त्वचा में रूखापन आ सकता है।
रूखी त्वचा का उपचार घर बैठे किया जा सकता है। अगर आप भी अपनी रूखी त्वचा से परेशान हैं तो नीचे दिए हुए घरेलू नुस्खों का उपयोग कर सकते हैं। लेकिन अगर आपको पहले से त्वचा संबंधित किसी भी तरह की कोई समस्या है तो त्वचा विशेषज्ञ से परामर्श करने के बाद ही इन नुस्खों का इस्तेमाल करें।
त्वचा में रूखापन दूसरी गंभीर समस्याओं के कारण भी हो सकता है। ऐसे में आपको ऊपर दिए गए घरेलू नुस्खों का इस्तेमाल करने से पहले त्वचा विशेषज्ञ से अवश्य परामर्श करना चाहिए। बिना डॉक्टर से परामर्श किए इन नुस्खों का इस्तेमाल करने पर आपको फायदा होने के बजाय दुष्प्रभाव भी हो सकता है।
अगर घरेलु नुस्खों से आपके रूखी त्वचा में कोई फायदा नहीं होता है या त्वचा का रूखापन समय के साथ बढ़ता है, कुछ समय के बाद त्वचा फटने लगती है, रूखी त्वचा में खुजली, जलन और दूसरी समस्याएं होती हैं तो आपको जल्द से जल्द त्वचा विशेषज्ञ से परामर्श करना चाहिए।
आपकी त्वचा के सूखने के कई कारण हो सकते हैं जैसे कि त्वचा के अनुरूप साबुन, क्रीम, लोशन या दूसरे उत्पादों का इस्तेमाल न करना, त्वचा संबंधित किसी बीमारी से पीड़ित होना, शरीर में विटामिन ए और डी की कमी होना, प्रदुषण के संपर्क आयना आदि।
कुछ विशेषज्ञों का कहना है कि ज्यादा देर तक नहाने से त्वचा का प्राकृतिक तेल ख़त्म हो जाता है जिसके कारण त्वचा में रूखेपन की शिकायत हो सकती है।
जोड़ शरीर के महत्वपूर्ण अंग हैं जो हमारे दैनिक जीवन की गतिविधियां जैसे कि उठना, बैठना, सोना, चलना आदि में महत्वपूर्ण भूमिका निभाते हैं। लेकिन कई बार कुछ स्थितियों के कारण जब शरीर के जोड़ जैसे कि कोहनी, घुटना, टखना, कंधा, कूल्हा आदि में दर्द होता है तो हमें अपने दैनिक जीवन के कामों को पूरा करने में काफी कठिनाइयों का सामना करना पड़ता है।
आमतौर पर बूढ़े लोगों में जोड़ों के दर्द की शिकायत होती है, लेकिन चोट, मोच या किसी बीमारी के कारण यह बच्चों या जवान लोगों में भी देखने को मिल सकता है। आइए, इस ब्लॉग में हम जोड़ों में दर्द के कारण, लक्षण और उपचार के बारे में विस्तार से जानने की कोशिश करते हैं।
Table of Contents
जोड़ों में दर्द के अनेक कारण हो सकते हैं जिसमें गठिया, बर्साइटिस और मांसपेशियों में दर्द आदि। जोड़ों में दर्द के मुख्य कारणों में निम्न शामिल हो सकते हैं:
ये भी पढ़े: घुटने में दर्द का कारण, लक्षण और घरेलू इलाज
आमतौर पर जोड़ों में दर्द और गठिया के लक्षण लगभग एक जैसे हो सकते हैं। उदाहरण के तौर पर, इन दोनों स्थितियों में निम्न लक्षणों को अनुभव किया जा सकता है:
गठिया होने पर आप दूसरे भी लक्षणों को अनुभव कर सकते हैं जैसे कि जोड़ों में सूजन आदि। हालाँकि, ये लक्षण अन्य अंतर्निहित स्थितियां जैसे कि ल्यूपस, सोरायसिस, गाउट या कुछ संक्रमण के कारण भी हो सकते हैं जिसकी पुष्टि जाँच के बाद होती है।
ये भी पढ़े: यूरिक एसिड बढ़ने का कारण, लक्षण, इलाज और आसान घरेलू नुस्खे
जोड़ों में दर्द का उपचार उसके कारण, प्रकार, गंभीरता और मरीज की उम्र एवं समग्र स्वास्थ्य पर निर्भर करता है। अगर जोड़ों में दर्द का कारण चोट है तो शुरुआती उपचार के तौर पर डॉक्टर आराम करने का सुझाव और सूजन के लिए कुछ दवाएं निर्धारित करते हैं।
दर्द को नियंत्रित करने के लिए दर्द निवारक या दूसरी दवाओं की आवश्यकता हो सकती है। साथ ही, शारीरिक चिकित्सा की भी जरूरत पड़ सकती है। इन सबके अलावा, जोड़ों के दर्द का इलाज करने के लिए डॉक्टर निम्न का इस्तेमाल कर सकते हैं:
आपके जोड़ों के दर्द के लिए सटीक उपचार क्या है – इस बात की पुष्टि जोड़ों के दर्द का निदान करने के बाद होती है।
ये भी पढ़े: हड्डी का कैंसर: प्रकार, कारण, लक्षण और उपचार
जोड़ें शरीर का महत्वपूर्ण हिस्सा हैं जिनकी गतिशीलता हमारे दैनिक जीवन की गतिविधियों को आसान और आरामदायक बनाती हैं। लेकिन अनेक कारण जैसे कि चोट, संक्रमण या बीमारी के कारण जोड़ों में दर्द की शिकायत हो सकती है।
जोड़ों में दर्द होने पर आपका चलना, फिरना, उठना, बैठना या दैनिक जीवन के कामों को करना मुश्किल हो सकता है। इस स्थिति में आपको जल्द से जल्द डॉक्टर से परामर्श करना चाहिए। डॉक्टर कुछ जांच की मदद से जोड़ों में दर्द के सटीक कारन का पता लगा सकते हैं।
उसके बाद, उचित उपचार से इसे दूर कर सकते हैं। जोड़ों में दर्द का उपचार कई तरह से किया जाता है। आमतौर पर जोड़ों में दर्द की समस्या को दूर करने के डॉक्टर दर्द के कारण, प्रकार, गंभीरता और मरीज की उम्र एवं संपूर्ण स्वास्थ्य को ध्यान में रखते हुए उपचार के प्रकार का चयन कर इलाज की प्रक्रिया शुरू करते हैं।