Filter :
The keto diet has gained massive popularity in recent times. While there is little research on the ideal duration, studies suggest that the keto diet can work in weight loss. Hence, the keto diet can essentially point towards your first steps to eating clean.
Before we learn how to do the keto diet, let us understand the mechanism behind it.
Carbohydrates burn down in the body to produce glucose, the primary source of energy. The general idea behind the keto diet is to reduce glucose levels in the body and substitute them with fat.
The fat would be converted to ketones, a clean source of energy for your body. This, in turn, would stabilise your blood sugar levels and effectively bring down your overall weight.
When your body is fuelled by ketones, instead of glucose, you tend to feel more energised, have fewer hunger pangs, and also reduced mood swings. However, keto is not just about lowering your carbohydrate intake and substituting it with fat.
Here are some things you must know before you start this regime.
An ideal keto diet plan for beginners must include a healthy dose of fat. You must look for heart-healthy variants of unsaturated fats like olives, cottage cheese, nuts, avocado, eggs, and seafood like salmon. Substitute your rice, bread, and pasta with healthier substitutes like non-starchy greens and lean meat.
Keto diet should not become an excuse to eat loads of processed fat. Processed food comes loaded with complex sugar and a high level of carbs. Focusing on cleaner fats that are whole and unprocessed is pivotal to get the desired results.
The best way to begin your keto diet is to know everything about it. Read reliable sources online on how to start a keto diet and learn about all the associated benefits and risks. Talk to friends and family members who practice the diet to understand how it will impact your current lifestyle.
Analyse and read if you would be able to manage the regime without any glitch.
Understand from your medical practitioner if this diet plan would be ideal for you. Sometimes a specific medical condition, dietary restriction, or medication can render you unsuitable for this diet plan.
Some conditions are:
You can design a simple keto diet menu for beginners with the staples you have in your home. Make a diet chart with the required calorie count and stick to it to ensure desired results.
Ensure that you don’t have many cheat days as even one cheat day can pull you very far from your goal.
The biggest challenge in this diet regime is to keep replenishing the electrolytes in your body. When you start a keto diet, you tend to urinate more often and can easily fall prey to dehydration.
Ensure that you have lots of fluids at regular intervals and also consume enough electrolytes like sea salt to maintain a healthy level.
The key to a successful keto diet for beginners is to eat right. Often the main reason to start a keto diet is weight loss. To avoid any health risks, ensure that weight loss is a slow and steady process.
Sudden and drastic weight loss can be detrimental to your overall health and can even prove fatal. You need the right amount of macronutrients along with the regular intake of fats.
Protein is an essential part of your meal. However, too much of it can hinder your ketone production. Generally, a keto diet menu for beginners should have around 20-25% Proteins, 70-75% of fats, and less than 5% of carbs.
You can try a protein supplement like Gradual protein powder that has a Gradual Release Energy System (GRES).
When your body starts keto, it will take time to adapt to it and initially may resist the diet. In this case, you might show flu-like symptoms.
There would be episodes of fatigue, nausea, joint pain, and mental fogginess during the initial few days.
Be patient and persistent as these would go away after a while. You can manage these symptoms effectively by doing the following:
From the day you start the keto diet, your meal chart would look utterly different from that of your other family members. You must keep them updated about your diet plan and ensure that they understand everything about it.
While you might get back to your regular diet eventually, they must be on the same page as you and know your restrictions.
Keto is a successful way to lose weight, but it might not work for everyone. You must track your progress and look out for any red flags. See if you feel better physically and mentally after following this regimen for a week.
Measure your weight daily and get your blood work analysed by your medical practitioner. You might want to download a reliable ketone tracking app for yourself to get started.
Keto is not a forever plan, and you must get back to your usual routine after a while. However, some people make changes to their lifestyle and adopt a healthier diet plan after trying keto. Your change must be a gradual and steady process.
Avoid suddenly switching to your regular dietary pattern. This will only promote unhealthy weight gain and negate any positive effect the keto diet had on you.
It is incredible to see how a keto lifestyle can do wonders for your overall health. However, if done recklessly, a keto diet plan can also pose significant health risks. Get your diet plan approved by a practising dietician before you start the keto diet.
Seek medical assistance if you experience:
Social conditioning has led to the term “breast cancer” being associated with women. According to a survey, the number of women undergoing breast cancer tests is almost triple the number of men.
But the fact of the matter is that breast cancer affects men, too. Either way, getting diagnosed with cancer is heartbreaking. Thus, the support of loved ones holds immeasurable value to a cancer patient.
As a family member, you may wonder how to cope when a loved one has cancer. You may be caught in a dilemma as to how you ought to behave and what you should do to help them.
Remember that every person is different. It is not for you to decide how they should get on with this life-altering condition. Instead, you need to be their pillar of strength.
Trying times like these call for being open with your loved one. Ask them how involved they want you to be.
Some people would rather deal with this diagnosis by themselves or with select family members. It doesn’t help anyone if you are butting in where you are not needed.
It is much better to openly talk about their state of mind and avoid misunderstandings from the very beginning.
Anything involving medical tests and frequent visits to the hospital can be nerve-wracking. Depending on the stage of cancer, the treatments may vary. Maybe your family member just needs someone with whom to discuss the options available.
So be their sounding board. Help them choose the path they feel most certain about, without imposing your thoughts on them.
People have a habit of taking to the internet every time they have a health-related query. Dissuade your loved one from doing the same. The internet is not the most credible space for medical advice.
Reading incorrect information can cause more harm than you’d realise. Help them understand that making an appointment with an oncologist is a far better decision.
Sometimes, to console a breast cancer patient, you just need to be by their side. Offer to accompany them to the hospital for the consultation and the subsequent treatment days.
The environment in hospitals is already grim. Your family member shouldn’t have to feel like they are alone in this.
As a person who is caring for them, you can also speak to the oncologist yourself. This shows that you are attentive to your family member’s needs and willing to support them in your limited capacity.
Chances are, your family member is already being subjected to a lot of breast cancer advice. What you can do differently is help them with their dietary routine.
Cancer treatments can lead to side effects that might disrupt their eating habits.
Moreover, it may also require the patient to eat foods with certain revitalising nutrients. Ask them what they feel like eating and if they’d want you to step in with grocery shopping or cooking.
A protein-rich spread on the table can go a long way in energising your family member.
Lending help is one thing. But becoming overprotective can be detrimental to the mental health of a cancer patient. Coping when a loved one has cancer is challenging, and may make you go overboard with suggestions and care.
This may cause your family member to feel like they are incapable of doing anything by themselves.
Don’t suffocate them with your constant breast cancer advice and assurances. Draw a line between being reliable and hovering around them all the time.
Knowing how to console a patient is not an exact science. Some things work, and others don’t. But almost always, patients crave a sense of normalcy.
They might prefer some aspects of their life to be untouched or unchanged by their medical condition.
Students might want to work on their assignments, and fathers might want to pitch in with household chores. Don’t admonish them for doing so.
Carry on with your life as you would and also encourage them to go about with theirs as much as possible. Do not let your conversations with them be weighed down by the diagnosis.
Even if you’ve wrapped your mind around how to help someone diagnosed with cancer, it doesn’t mean that all your other family members have gotten the memo.
They may not know how to cope when a loved one has cancer and might make the patient feel like an invalid with their behaviour.
Of course, they mean well. But it can come across as overbearing to the person battling cancer and may even result in needless animosity among family members. So intervene if you can and shed some light on the situation.
Help everyone understand cancer from the perspective of your loved one going through this difficulty.
No matter what’s said and done, there’s only so much you can do as a family member to console the patient. Your loved one may better be able to relate to someone who is suffering from cancer just like they are.
Joining a support group can be a positive move for their mental health. It may even make the journey of recovery more bearable.
Family members still learning to cope when a loved one has cancer also benefit from support groups.
Your role in the life of a person going through cancer depends greatly on their outlook towards life. Along with breast cancer advice, have a heartfelt talk with your oncologists and counseling team.
They may guide you in alleviating some of the stress and pain that your family member is going through.
To help someone diagnosed with cancer, you need to be supportive, open-minded and understanding. That is what matters the most.
For new mothers-to-be, the last trimester of their pregnancy can be a period wrought with mixed feelings. On the one hand, there is the increased exhaustion, and then there’s also the eager anticipation of getting to hold their baby.
It is only natural that they would have plenty of questions about the upcoming childbirth. While it is up to the mother to choose between a natural delivery and cesarean delivery, correct information regarding the risks and benefits associated with the procedures will help her make the right decision.
Here’s some information about the natural way of giving birth:
Table of Contents
A normal delivery occurs when the mother goes into labor either spontaneously or with the help of drugs and/or other techniques. Most types of normal delivery do not involve a surgical procedure as the infant is passed through the birth canal.
Also known as a vaginal delivery, this process may include the use of instruments and has far fewer complications than a c-section.
It is the safer option for an infant and also increases the chances of your subsequent pregnancies being free of risks.
Weight control is a crucial factor that can increase the probability of you having a normal delivery. Women who are overweight or obese are likely to have infants who weigh more than the average. In such a case, the obstetrician might recommend a c-section.
Going through labor and enduring natural childbirth requires substantially more resilience on the part of the mother. Increased stamina and endurance can aid normal delivery.
Doctors giving advice for normal delivery often state that the position of the baby is what determines whether a normal delivery is suitable or not. When the infant has an anterior position, i.e., his/her head is facing downward, and towards the spine, it is highly preferred.
There are a few ways to encourage such positioning. Read the next section for some normal delivery tips.
One of the things to do for normal delivery is to ensure that you adopt some new lifestyle practices. This includes dietary changes, regular exercise, changes in sleeping and resting positions, etc.
These are some of the signs of normal delivery:
One of the normal delivery symptoms is a feeling of increased pressure in the uterus. This marks the beginning of the labor period, and once your contractions become more regular, you are well into the first stage of natural delivery.
As the fetus is about to be pushed out of the birth canal, you may feel the urge to urinate since the pressure has shifted onto your bladder. The same holds true for your bowels. Hence, women are asked to have an empty stomach before the process begins.
You may experience sudden changes in energy levels. This is due to the release of adrenaline into the blood. It is your body’s way of aiding the childbirth by giving you the boost you need to push through.
As you may well know, the amniotic sac is what holds the fetus. When you are ready for the delivery, this sac breaks and the liquid spills out. This is more commonly known as water breaking.
The possibilities of normal delivery vary from person to person. But so far as there are no pre-existing medical conditions that necessitate a cesarean, it is better to opt for a natural delivery.
There are several reasons for this.
The process of normal delivery has three stages:
In the labor phase, the cervix should soften and stretch. Once the cervix is completely dilated, the uterine contractions enable the infant to pass through the birth canal.
On the whole, it lasts around 36-48 hours if there is no surgical incision involved. In contrast, a c-section can go on for 72-108 hours as both the child and mother get hospitalized for a longer duration.
In the year 2018-19, as many as 33.80% of childbirths at private facilities were a result of caesareans, according to a report by the Ministry of Health and Family Welfare in India. That is an alarmingly higher rate in comparison to the normal standard of 10-15% set by the World Health Organization.
No expecting mother should go through such a beautiful phase of life without expert guidance. Visit CK Birla Hospital and consult our obstetrician to decide a path that is best for you and your child.
Breast cancer is one of the most prevalent cancers among Indian women. As per a 2019 report published in NCBI, breast cancer constitutes more than 30 per cent of all cancers in females.
The survival rate largely depends on early diagnoses and the right treatment.
Breast tumour size is an important factor in determining breast cancer stage but not the only one. Other factors like the location of the tumour, how much it has spread, hormone receptor status also play a significant role in deciding the stage of breast cancer.
Doctors use various tests and examinations to evaluate the specific characteristics of a person’s breast cancer while determining breast cancer stages.
Table of Contents
The diagnostics tests and scans of the person help the doctors in tumour staging. The TNM staging system is a commonly used tool to describe the stage.
Combined results are used to determine the stage of cancer for each person.
Tumour size is generally measured in millimetres (mm) or centimetres (cm). A number suffixed with T tells you the main tumour’s size. Higher the number, larger is the tumour and its spread.
The American Cancer Society uses this particular system for tumour staging:
TX – The primary tumour cannot be evaluated
T0 – No evidence of cancer in the breast
T1 – The tumour detected is less than 20 mm in size. It further has four sub-stages categorized as per the size of tumour:
T2 – When the tumour is larger than 20 mm but smaller than 50 mm
T3 – When the tumour is larger than 50 mm
T4 – The tumour has grown into the chest wall and/or skin. It also includes inflammatory breast cancer.
The N value of the TNM staging system assesses whether cancer has spread to the nearby lymph nodes. The doctor generally takes the sample from the armpit area called the axillary lymph nodes and graded through the following:
When cancer cells have spread to distant organs or tissues of the body, it is metastatic breast cancer. The most common metastatic areas are the liver, bones, and lungs. The assessment is as follows:
MX – Unable to evaluate the distant spread
M0 – No evidence found for cancer spreading to distant parts
M1 – Cancer has spread to distant parts
Breast tumour size is one crucial determinant of the cancer stage along with lymph node and metastatic status.
However, some other deciding factors that doctors use to evaluate breast cancer staging are:
Knowing the hormone receptor status is essential in tumour staging and also deciding an effective breast cancer treatment plan. For this, the doctors evaluate the breast cancer cells for specific proteins that are estrogen and progesterone receptors.
The cancer cells often attach themselves to these hormones and feed on them to grow.
Hormone therapy is generally the most effective treatment in such cases. It prevents estrogen and progesterone from attaching themselves to the receptors, thereby keeping cancer from growing and spreading.
One of the newest determinants to be incorporated into breast cancer staging is HER2 status. HER2, i.e., human epidermal growth factor receptor 2, is a gene that can play a role in the development of breast cancer.
HER2 receptors are proteins that control how a healthy breast cell grows, divides, and repairs itself. Doctors test HER2 status to see if there are higher than normal levels of this receptor and then term it as HER2 positive cancer.
Targeted therapies generally work best in such cases.
This is known as breast cancer grading. In this, the breast cancer cells are carefully observed under a microscope for their appearance.
The ones that look quite similar to normal cells are considered to be slower growing. Contrarily, the ones that look very different will probably grow and spread faster.
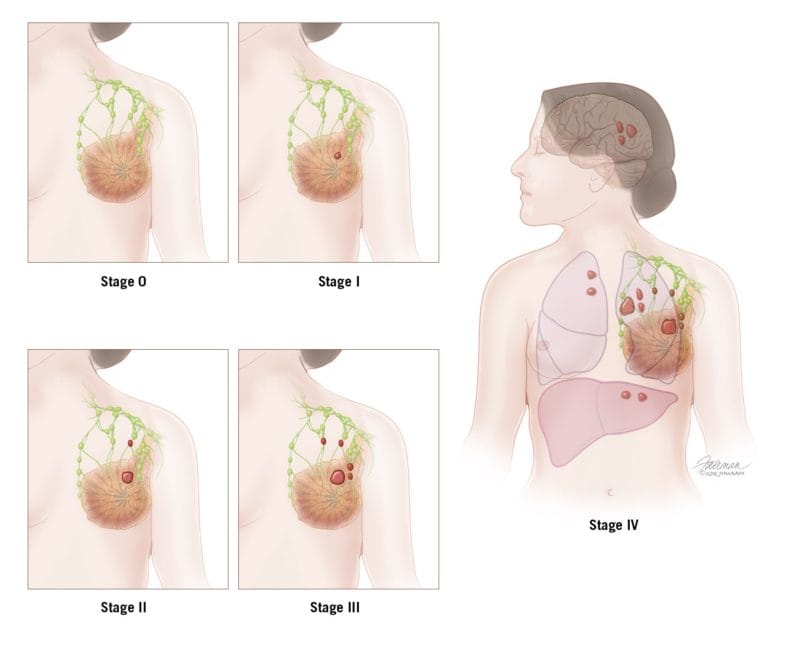
Depending on the stage of breast cancer, age and general health of the patient, your doctor will prepare a treatment plan.
Options include:
Every person’s breast cancer is different. The tumour staging helps in evaluating the extent of cancer present and deciding the best suitable treatment option for it.
Breast tumour size is undoubtedly the most important deciding factor for breast cancer staging. Early diagnosis holds the key to the efficient and effective treatment of breast cancer. It is important to consult your doctor right away whenever you feel you show any signs or symptoms of breast cancer.
According to the latest stats, over two million individuals have been infected with the novel coronavirus in 182 countries and territories across the world. In India, four deaths and 166 confirmed cases have been reported until now.
In his address to the nation on 19th March 2020, Prime Minister Modi has urged everybody to stay at home unless it is absolutely necessary to step out and follow social distancing protocols. In the wake of the global pandemic, over 13 countries in the world, including India, have closed down schools and colleges. Many individuals have been asked to work from home – which is a prudent step to contain the infection from spreading through unnecessary contact.
The novel coronavirus disease is surface borne and can remain on contaminated surfaces for up to 24-hours. This means that work desks, printers, keyboards, etc., can remain infected for hours unless properly disinfected and can be a key source for spreading the infection. Besides, most employees work in closely situated cubicles or open floor plans. Thus, the social distancing of six-feet between individuals is often not possible, making everybody in the office susceptible to the disease.
To contain the spread of the virus, the government has requested various organisations to allow their employees to work from home. This will allow employees to avoid unnecessary travel and close contact between people.
Top Indian firms like Infosys Ltd., Hindustan Times, Zerodha, and various law firms have allowed their employees to work from home to ensure business continuity without compromising on the health of their employees. Some of these companies already had contingency plans in place. But many had to rush-in to create and implement sustainable and secure work from home policies – which is a commendable feat.
Work from home is an excellent option to prevent the spread of coronavirus in the country. Now, you can finally live the dream of working in your pyjamas! Yet, cruel as it may sound, the picture isn’t as rosy in real-life, especially if you have kids (with their schools shut down) frolicking at home.
But don’t worry – there’s a way out of every situation. To help you out, we have compiled a list of things you need to stay productive while working from home:
Apart from the tips mentioned above, make sure that you avoid unnecessary outings and social gatherings. It is also recommended that youngsters don’t mingle with the elderly to prevent the spread of the novel coronavirus disease.
If all of us can maintain proper hygiene and follow social distancing for the next few weeks, we can beat the coronavirus and come out of this stronger and wiser. Meanwhile, if you feel you are coming down with a fever or flu-like symptoms, contact a doctor or click here to book an urgent appointment at CK Birla Hospital.
Chemotherapy or chemo is the most commonly adopted procedure to treat cancer. Cancer is the uncontrolled growth and spread of abnormal cells, which causes a person to be severely ill.
The later cancer is detected, the more the chances are for it to prove fatal.
Chemotherapy is a drug therapy that works by killing these cancer cells to either cure the person or to control further growth. Unlike radiation therapy or surgery, which target specific areas, chemotherapy procedure works on the entire body.
However, in the process of killing the cancer cells, chemotherapy often also affects the healthy cells resulting in some undesired side-effects of this treatment.
Table of Contents
Depending on the type and stage of cancer, chemotherapy is used to:
Chemotherapy uses drugs in a decided dose and administered to the affected person in a suitable method. The drugs used in chemo treatment are potent and thus need to be used carefully. The treatment may be given in various ways:
Oral and topical treatments are easily performed at home, while others are usually performed in a hospital or a cancer treatment centre.
For greater effectiveness of the cancer treatment, chemotherapy is often used in combination with other treatments like:
Chemotherapy is a cyclic treatment which is performed in intervals so that normal cells in the body have time to recover from its side-effects. Sometimes doses may be given one day or a certain number of days in a row, followed by the rest period, then after a week or every other day.
Depending on the drug and the treatment response on the individual, its respective cycle is decided.
Before proceeding with the chemotherapy procedure, your healthcare specialist carefully plans the drug(s), their dose, and the treatment schedule. The preparation process takes into consideration the type of cancer, its stage, and what will suit you best.
Your doctor may require you to get some blood tests done to be sure of your underlying health as it can affect the effectiveness and duration of the treatment. If there’s a problem, your doctor decides your treatment accordingly.
Doctors also discuss the first chemo treatment side-effects so that you’re informed and can prepare yourself. For instance, the chemotherapy process often brings infertility as a side-effect, so your doctor might suggest you preserve your sperm or eggs for use in the future.
The effects after the first chemo treatment greatly vary from person to person. How the body will respond to the treatment will depend on various factors:
Since every person responds to the treatment differently, your oncologist can seldom tell you exactly how you will feel during the chemotherapy procedure.
Usually, it’s perfectly alright to continue working during chemotherapy as long as you can match the treatment schedule along with your health.
Several companies have laws in place for such employees. Depending on the job you do, you can ask for a part-time or a work from home option from your employer on the days you feel a little sick. You can learn about these laws online or a reliable source.
Although a very useful treatment for cancer, chemotherapy isn’t free of probable adverse effects. The healthy cells that are often targeted by chemotherapy drugs along with the cancer cells, sometimes begin to show abnormalities in some individuals. However, in some cases, most side-effects are known to go away once the complete treatment is over.
The common side-effects of aggressive chemotherapy are:
Some people may also experience other side-effects like anxiety and mental health problems. It’s important to talk to your doctor from time to time whenever you show any sign as most of them are treatable concerns.
Cancer is a life-threatening condition which not only affects you physically but can also exhaust your emotional capabilities. It’s very natural to be insecure, to have a lot of questions in mind, and to feel sad and depressed. But instead of letting this pull you down, you must consult a reliable healthcare provider who will guide you correctly through this difficult phase of life.
You can also consider talking to a certified counsellor who can help you stay positive and hopeful in all situations. A mindful conversation with your family and loved ones who will stay by your side come what may is a sure way to lift your spirits and get you going.
The gallbladder is a four-inch organ located in the upper-right area of the abdomen, under the liver. It helps produce, store, and transport bile, a yellowish-brown fluid produced by the liver.
This fluid is responsible for digesting and breaking down food with fats.
When problems arise, if first-line treatments do not work, and the issue is persistent, doctors may recommend removal to prevent further complications.
Though the gallbladder is a component of the biliary system, it is not considered to be an essential organ. Bile fluid can find it’s way directly to the small intestine through ducts in the liver.
Table of Contents
The procedure for removal of the gallbladder is called Cholecystectomy. Two types of procedures come under cholecystectomy:
This is the most common choice of surgery used to remove over 95% of gallbladders. This method is less invasive and entails 3 to 4 small incisions.
The procedure involves the use of a small tube through the incision. This tube holds a camera (called a laparoscope) along with surgical devices.
The surgeon extracts the gallbladder through one of the incisions.
A conventional method that involves making a single large incision at the site and extracting the gallbladder through it.
There could be many reasons to opt for gallbladder removal. There could be blockages due to bile being thick or even deposits of hard substances known as gallstones.
Mostly, these gallstones pass naturally. Your doctor may recommend surgery if there is notable pain or larger stones.
Other reasons for cholecystectomy could be:
Common factors that could increase the risk of gallbladder problems are:
Gallbladder removal is a low-risk and frequently performed surgery. While any form of surgery has threats, the risk of not having the procedure when recommended could be far worse.
Some of the possible gallbladder removal complications could be:
Above are general risks of a cholecystectomy procedure. However, each individual may face different risks depending on their history and body composition.
Disclose your complete history to your doctor and discuss any fears about complications that may arise.
If you smoke, let the surgical team know and plan on quitting before the surgery to decrease the risk of complications.
If you have a laparoscopic cholecystectomy, you would mostly be discharged the same day. An open cholecystectomy may need you to stay overnight for monitoring.
While your doctor will give you a comprehensive download, here are some things to keep in mind:
You would be placed under anaesthesia, the surgery would be conducted, and if needed, fluid might be drained.
The surgeon will make incisions after anaesthesia. Carbon dioxide will be used to inflate your abdomen for easy visibility of organs.
Once the procedure is complete, the gas is let out through the incisions.
The following are common symptoms to watch out for:
Depending on the reason for surgery, the benefits may vary, but the general advantages of gallbladder surgery range from the following:
If you experience any of the above symptoms.
It is important to follow the instructions given by your doctor. Make sure to wash your hands and sterilize whenever caring for the wound. Avoid wearing tight clothing that might restrict the healing of the wound.
Patients usually take up to 3 weeks to return to normal activity. So, slowly increase your activity level and avoid abrupt exercises.
Maintain the health of your biliary and digestive system by eating right and keeping fit. Ensure to add nutritious high-fibre food like fresh vegetables and whole grains.
Avoid eating high-fat meals and processed food to prevent overloading your system. Drink 8 to 10 glasses of water daily to stay hydrated.
While the prevention of diseases with a healthy lifestyle should be your first priority, the cure for them is also advancing rapidly. If you have experienced any of the symptoms stated for a prolonged period, or are continually facing gastrointestinal issues, make sure to visit a doctor promptly.
Folic acid plays a vital role in the growth and development of your baby, especially in the first trimester of pregnancy.
Hence, folic acid supplements are often prescribed during pregnancy. Let’s explore the importance of folic acid during pregnancy.
Table of Contents
Folic acid, also called pteroylmonoglutamic acid, is the synthetic form of Folate (Vitamin B9). While folate is typically found in leafy vegetables, folic acid is present in fortified food items or supplements.

Doctors normally prescribe folic acid for pregnancy as it facilitates cell growth, production of red blood cells, and DNA formation. Thus, women who are pregnant or trying to get pregnant should start consuming folic acid daily before conception and must continue for at least three months after.
As stated earlier, folic acid aids the production of new cells. Naturally, when you are expecting, your body is dedicated to generating more cells for the baby’s development. Folic acid benefits the body as it helps in the creation of proteins, which form the building blocks of cells.
Here are the folic acid benefits for your baby’s developmental health:
Typically, the neural tubes develop into the spinal cord and brain by the 28th day since conception.
However, if the neural tubes fail to close properly, it results in a condition called neural tube defects (NTDs). The most prevalent forms of NTDs include:
Babies suffering from anencephaly may not survive, while those with spina bifida and encephalocele may struggle with a permanent disability.
Therefore, it comes as a relief that one of the greatest advantages of folic acid in pregnancy is that it prevents NTDs in babies.
In fact, it may cut down the risk of NTDs by an impressive 70%!
Congenital heart defects (CHDs) are abnormalities arising out of the underdevelopment of heart or nearby blood vessels before birth.
These developmental defects could adversely affect the heart, heart valves, arteries, and veins. Studies indicate that folic acid supplementation before pregnancy can reduce the risk of CHDs.
Folic acid can prevent structural anomalies and defects as it regulates homocysteine metabolism. As a result, it can prevent oral clefts in the lip or the palate.
Folic acid supplementation also inhibits uterine contractions, which could otherwise result in preterm birth (PTB) or miscarriage. PTB is a significant cause of neonatal mortality and morbidity.
Folic acid decreases the risk of developing anaemia during pregnancy, gestational diabetes, and other birth-related complications. Nearly 5% of women register a haemoglobin count that is less than 11.0g/dL, which is an indicator of anaemia.
The body requires folate, cobalamin (vitamin B12), and iron to produce more red blood cells. Hence, supplementing folic acid and vitamin B12 could bring down the chances of developing anaemia.
Similarly, folic acid supplementation can cut down the risk of developing gestational diabetes by 22% (for 400mcg supplements) and 30% (for 600mcg supplements).
Additional benefits of folic acid supplementation for pregnant women involve lower rates of placenta-related pregnancy complications.
This is because folic acid can regulate trophoblast invasion, which ensures regular implantation and placentation during gestation.

Ideally, the prescribed folic acid pregnancy dose is a minimum of 400 micrograms (mcg) per day.
However, a woman should typically consume about 600mcg of folic acid from all sources, including food and vitamin supplements.
Some women may be specifically advised to take folic acid supplements during pregnancy as their baby may be at higher risk of NTDs.
Mainly, this includes women who:
Folic acid admittedly has a few side effects. Certain individuals may find it hard to convert folic acid in the active 5-MTHF form.
As a result, their blood levels indicate a high concentration of unmetabolised folic acid. Chronically elevated levels of unmetabolized folic acid could increase cancer risk and vitamin B12 deficiency.
A study conducted in 2016 highlighted how women with high folate levels could birth a child with an autism spectrum disorder.
Adopting a healthy diet can supply naturally occurring folate to the body, alongside essential nutrients like calcium, fibre, and vitamins A and C.
Here are a few natural food sources of folic acid for intake during pregnancy:
Now that you understand the link between pregnancy and folic acid, you are in a better position to include it in your daily routine. It is an essential vitamin right from conception until you stop breastfeeding your child.
However, before you begin supplementation, it is wise to get your doctor’s opinion on the matter. To determine the correct folic acid dosage and any other pregnancy-related concerns, visit our specialists at CK Birla Hospital.
India is fighting an arduous battle to contain the spread of novel coronavirus disease. According to the latest stats released by the Ministry of Health and Family Welfare, as of 21 March 2020, a total of 298 COVID-19 cases have been reported in 22 states/union territories of India. Out of this, 23 patients have been cured, one has migrated, while four succumbed to the disease.
Table of Contents
Washing your hands regularly for a minimum of 20 seconds and avoiding contact with contaminated surfaces are the best methods to keep yourself from contracting the disease. Apart from these precautions, self-quarantine has also been recommended to all citizens of India.

India has been able to manage the outbreak until now with only a few reported cases. However, it is suspected that we are currently in the third stage of the pandemic, which means the number of infected people will multiply exponentially shortly unless we take proper precautions.
In light of this situation, the central and state governments have set up additional labs for free coronavirus testing. Moreover, for the good of the public, they have updated the protocols for screening for COVID-19.
Quarantines are generally used by governments to prevent the spread of contagious diseases. Quarantine is meant for people who do not have any symptoms of the disease but have been exposed to the sickness. This group of people includes relatives of patients, caregivers, friends, etc. Quarantine, however, must not be confused with isolation. Isolation is a precautionary measure for individuals who are already sick to keep them away from those who are healthy.
Amid the pandemic outbreak, the responsible citizens of the country need to make educated choices for their own health, as well as of others. To prevent the spread of coronavirus disease, the Ministry of Health and Welfare has advised a self-quarantine of 14-days for anyone who:
Presently, there’s no legal sanction behind this recommendation. However, it is an important step that will go a long way in helping India win this fight against COVID-19.
All quarantines are not the same. However, if you are home-quarantined for COVID-19, we have compiled a list of dos and don’ts to help you complete your quarantine successfully without adversely impacting your mental and physical health.
Stay at one place – This is the most crucial aspect of your quarantine. Limit yourself to one, well-ventilated room and avoid contact with others. You should strictly not entertain any visitors at this time. Instead, spend your time doing something you never had the time for – such as painting or writing or even catching up with friends over the phone.
Avoid mass gatherings – A person under quarantine must not attend any weddings, funerals or religious functions. They must also stay away from the elderly, small children, those with compromised immunity and pregnant women.
Maintain proper hygiene – Do not swap plates, share food, or use common cutlery. Instead, eat in your room and wash your utensils properly before replacing them in the common area. You should clean and keep your utensils and laundry separate during this period.
Your dog is safe – Dogs and cats cannot transmit coronavirus, and there’s no reason to abandon them. However, if you are under quarantine, avoid kissing, petting or hugging your pets for a few days.
Wash your hands often – At the cost of sounding repetitive, we would once again reiterate the importance of washing your hands with soap for at least 20 seconds after you touch any surface and before touching your face or having meals.
Wear and change masks regularly – Wear a mask at all times and change it after every 6 to 8 hours. Used masks should be first disinfected and then burnt, instead of being directly disposed of.

There is a lot of wisdom in this age-old saying that prevention is better than cure. That’s why we urge you to take proper precautions and play your part in helping India fight this global pandemic. Here are some tips to stay safe from COVID-19: